ISSN : 2576-3938
Journal of Emergency and Internal Medicine
Palliative Care Trends and Challenges in Nigeria ÃÆâÃâââ¬Ãâââ¬Å The Journey So Far
Folaju O Oyebola*
Department of Pain and Palliative Medicine, Federal Medical Center, Abeokuta, Nigeria
- *Corresponding Author:
- Dr. Folaju O. Oyebola
Head, Department of Pain and Palliative Medicine
Federal Medical Center
Abeokuta
Nigeria
Tel: +234 809 594 8007
E-mail: fooyebola@yahoo.com
Received date: December 14, 2017; Accepted date: December 24, 2017; Published date: December 26, 2017
Citation: Oyebola FO (2017) Palliative Care Trends and Challenges in Nigeria – The Journey So Far. J Emerg Intern Med. Vol.1 No.2:17
Abstract
Nigeria is the most populous country in Nigeria with a population of 170-180 million people; the health system is “pay for service” for the majority of people. In recent times, with increase longevity the prevalence of chronic diseases that are life threatening requiring palliative care has escalated. Such patients compete for the limited available resources and bed spaces in the hospitals and often terms labelled as bed-blockers.
Keywords
Palliative care development; Chronic diseases; Gross Domestic Product (GDP); Life expectancy
Abbreviations
GDP: Gross Domestic Product; HPCAN: Hospice and Palliative Care Association of Nigeria; APCA: African Palliative Care Association; AGM: Annual General Meetings; ACS: American Cancer Society; FMOH: Federal Ministry of Health; PFHI: Partnership Project Tagged “Hospital Pain Free Initiative Project; FMCA: Federal Medical Center Abeokuta; WHO: World Health Organization.
Introduction
There is a gradual erosion of the hitherto extended family support and patients get isolated both at home and in the hospitals. The life expectancy is lower than in most of the developed countries with low Gross Domestic Product (GDP). The annual national budget for health is a ridiculous 1.5-3%, oscillating whenever the government changes (Figure 1).
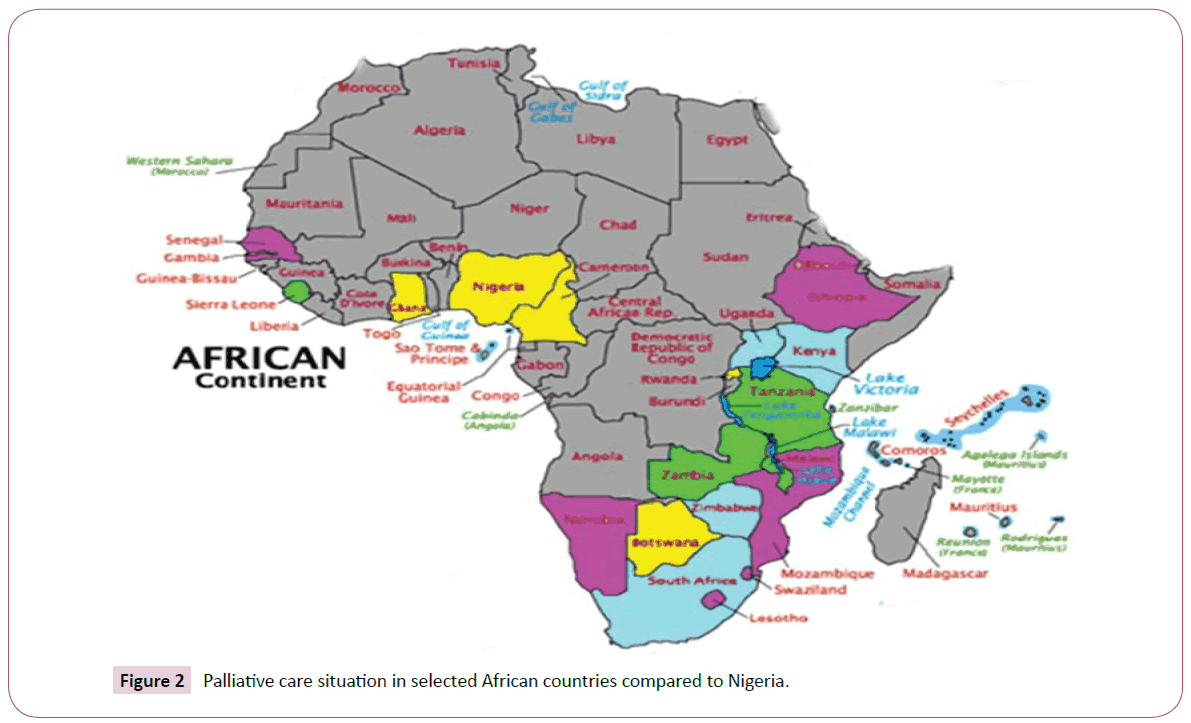
Palliative Care is still at a developmental stage in Nigeria despite decades of its introduction by Mrs. Fatunmbi and Dr. Anne Merriman in Nigeria in 1993. All efforts by the duo in terms of sensitization and advocacy to the then Government proved abortive, as Dr. Merriman had to move to Kenya and later Uganda. It is obvious that what could have been a gain to Nigeria became the East Africa legacy Figure 2 and Table 1.
| Developmental stages in Nigeria | |
|---|---|
| Size | 923,768 square kilometers |
| Population | 170 m |
| Life expectancy | M:F 48.0; 49.6 |
| Per capital income/GDP | (US$) 640 |
| Prevalence of HIV/AIDS | 5.8% (2003), 4.4% (2005) |
| Prevalence of cancer | 100,000 new cases/annum |
| Palliative care burden | 4.6 million |
Table 1: Palliative care developmental stage in Nigeria.
It is equally worth acknowledging the roles of other International palliative medicine specialists like Dr. Jim Rodgers (BESOUK- 2003-2005 Project), Dr. Carla Alexandria and Dr. David Oliver (2008-2014) and Macmillan Nurses from UK supporting different Centers in the country.
Ironically, in 2007 it was the same Dr. Anne Merriman that facilitated the inauguration of the Hospice and Palliative Care Association of Nigeria (HPCAN) together with the national association founding fathers. The African Palliative Care Association (APCA) and Dr. Anne Merriman provided the seed grants to take-off the Association. Since then palliative care services have been scaled-up in at least 5 out of the 6 geopolitical zones in Nigeria. The HPCAN had liaised with the Federal Ministry of Health severally and in 2008 submitted a proposal for the establishment of Palliative care Units in all the tertiary health institutions in Nigeria and today we have about 15 of such Centers scattered across the nation.
Since 2007-2017, the HPCAN Annual Scientific Conferences and Annual General Meetings (AGM) have been held in the following states of the nation: Oyo, Kaduna, Anambra, Kwara, Rivers, Osun, Ogun, Benue and Abia states. The 2015 edition was organized by Dr. Oyebola and strategically co-hosted by a Federal Government tertiary health institution, State Hospital, Privately owned faithbased hospital and a privately owned University Teaching Hospital to involve secondary level of care and privately owned health facilities.
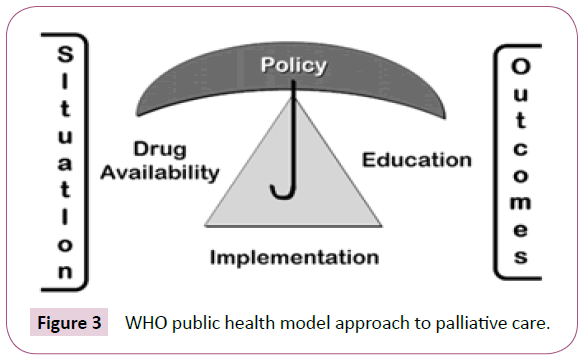
Using the WHO Public Health Approach to Palliative Care, Nigeria has made a significant achievement in palliative care development compare to most countries along the West Africa Coast (Figure 3).
Figure 3: WHO public health model approach to palliative care.
National Palliative Care Health Policy
Despite the prescriptions of the WHO in 2002 and its reemphasize at the 2004 WHO General Assembly that palliative care should be integrated into all nations health care system, several African countries including Nigeria are yet to approve it as a policy. However, the Nigeria government in 2006 set-up a Consultative Committee on Cancer and HIV/AIDS Policy draft which incidentally our palliative care champions participated and integrated palliative care into the draft. A decade after the white paper approving the policy is yet to see the light of the day.
This lethargy had contributed significantly to the slow level of palliative care development in Nigeria, as the palliative care practitioners have no access to the nation health budget. The HIV/AIDS patients fair better because of the global Grants funding their medications but unfortunately the Cancer and other life-limiting end-of-life-care patients have to cope with “pay for service” fees.
Institutional Policy and Implementation
In 2006, after Dr. Oyebola had a postgraduate training in palliative medicine at the famous University of Cape Town, South Africa being the first specialist to qualify in Nigeria. He submitted a proposal to his local hospital management requesting for a local policy approval to integrate palliative care into the existing acute care services. He pioneered palliative medicine in Nigeria and became the first full-time pain and palliative care physician by establishing the first pain and palliative medicine department at the Federal Medical Centre Abeokuta, Nigeria. This was the first Hospital-Based Palliative Medicine services and beginning of integrating chronic pain management, palliative and End of life care into an acute care hospital in Country. It is gladdening that the country today can boast of more than 15 similar facilities in Nigeria making use of their local institutional policies to move forward and hopefully the government would do the needful soon.
Education and Drug Availability
In a cross-sectional self-administered questionnaire based study carried out among health workers who attended the 7th Annual HPCAN Conference at Oshogbo, Osun state Nigeria. The questionnaire focused on the state of palliative care in Nigeria [1]. The information obtained from the questionnaires were coded, entered and analyzed.
Majority of the respondents claimed they do not have palliative care training during their basic training (Table 2).
| Variables | Frequency | Percentage |
|---|---|---|
| Yes | 17 | 34% |
| No | 33 | 66% |
| Total | 50 | 100% |
Table 2: Undergraduate palliative care training.
47% have formal training in palliative care while 53% have had ad-hoc training post basic. Though those professionals with formal palliative care training form the core HPCAN members. Almost all the respondents (92%) believed there is need to train palliative care specialists in Nigeria. 53% of the respondents had palliative care CME/training in the last 1 year and 48% did not have any (Table 3).
| Trainings | Frequency | Percentage |
|---|---|---|
| ADHOC Training | 9 | 53% |
| Formal Training | 8 | 47% |
| Total | 17 | 100% |
Table 3: Post-qualification palliative care trainings.
Forty-eight percent (48%) have had 1-3 local palliative care training, 14% have had 4-6 trainings, 10% had 7-9 trainings and 28% of the respondents had none. Twenty-six percent (26%) of the respondents have had 1-3 International palliative care training/conferences, 8% has had 4-6 international trainings and 56% had none. Sixty percent (60%) of the respondents admitted that they have no palliative care specialist in their centers, 34% had about 1-3 specialists while only 6% had about 4-6 specialists [2-4].
Majority of the respondents 38% had been in palliative care for 2-5 years while minority 8% had been in palliative care for up to a decade (Table 4).
| Years of Experience | Frequency | Percentage |
|---|---|---|
| Less than 2 years | 12 | 24% |
| 2-5 years | 19 | 38% |
| 6-10 years | 11 | 22% |
| >10 years | 4 | 8% |
| Total | 50 | 100% |
Table 4: Numbers of years in palliative care practice.
The estimated palliative care needs in Nigeria is well over 4.6 million saddled with severe dearth of manpower. There is an adage that “you can never give what you do not have”. So one of the big challenges is education and training for the teaming Nigeria health care professionals that are eager to be trained [5-9].
The few palliative care specialist doctors and nurses in the country had to make self-sacrifices to train in Uganda, South Africa and UK with their own personal money. At present these few specialists are fairly enough to constitute a palliative care faculty in the country hopefully with the support of other International faculties to start training [10].
Medication
Nigeria had no access to opioid medication for about 15 years and it was the efforts of the Pain Society of Nigeria, Palliative care group and African Palliative Care Association that influenced access to this medication in 2005. In view of the gap years many Nigerian health care practitioners trained within that period lack the skill to prescribe and administer Opioids to the patients (Opioid phobia).
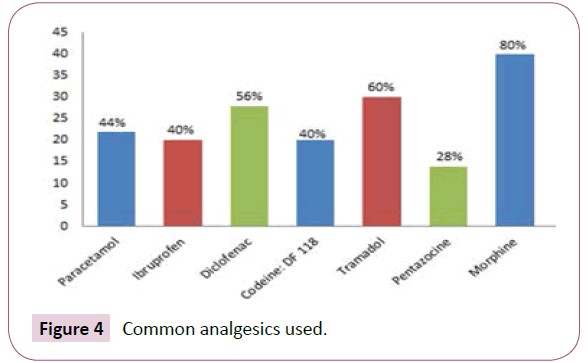
Morphine 80% is most commonly used analgesics used in palliative care services in Nigeria and is widely available in the country. Although most health care workers with inadequate training in pain management is Opioid phobia and feel more comfortable with Tramadol and Pentazocine (Fortwin) (Figure 4).
It was deduced by the respondents that 70% of the challenges facing palliative care practice in Nigeria is lack of government policy, while 68% attributed to lack of funding, 26% and 24% of the respondents attributed part of the problems to manpower and transportation challenges respectively.
Majority 74% of the respondents do not know of any exiting health policy supporting palliative care in Nigeria. Seventyeight percent (78%) of the respondents believed the health care system in Nigeria are not good enough for patient suffering from life-limiting illnesses, while only 8% believed it is good [2].
All of the respondents agreed that there is a need for palliative care in Nigeria and 94% of the respondents believed that hospice and palliative care facilities in Nigeria are inadequate.
The Opioids accessibility, prescriptions and dispensation had scaled-up in Nigeria with the American Cancer Society (ACS) – Federal Ministry of Health (FMOH) Partnership Project tagged “Hospital Pain Free Initiative Project (PFHI)”. Its mandate is to train all Nigerians Health Care Professionals in the skills and knowledge of pain management across Nigeria. With this project many Nigeria clinicians have been empowered especially at the tertiary health Institutions level. The hospital consumption of Opioids has escalated and opioidphobia among hospital staff and patients is gradually becoming a cruel past.
SWOT Analysis of the Current Nigeria Situation
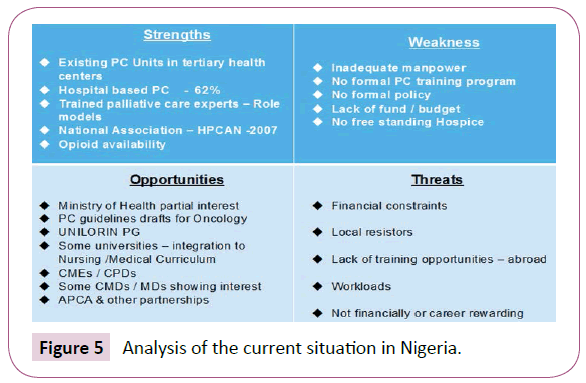
In recent past a significant and measurable achievement had been made to scale-up palliative care services at the tertiary health care settings. Many centers like Ibadan, Zaria and Abeokuta had been organizing ad-hoc education and trainings for Nigerians in conjunction with their foreign partners. The Ibadan group is working with the Hospice Uganda Africa and Dr. Anne Merriman. The Federal Medical Center Abeokuta (FMCA) collaborates with Dr. David Oliver of Kent University cum wisdom hospice and Ellenor-Lions Hospices in UK (Figure 5).
Only a handful of medical and nursing schools offer some few hours of palliative care teachings in Nigeria Universities. However, a small gain and step has been put in place at the University of Ilorin to commence postgraduate diploma in palliative medicine in a few years’ time. Most of these challenges are due to official bureaucratic procedures at the University Council and Professional bodies approval.
The FMCA further extended her empowerment of others by education, training and clinical placements for staff of some secondary level of health care facilities like State Hospital Ijaye Abeokuta and Sacred Heart Catholic Hospital Abeokuta. The latter now has a solid team and dedicated facility for palliative care services.
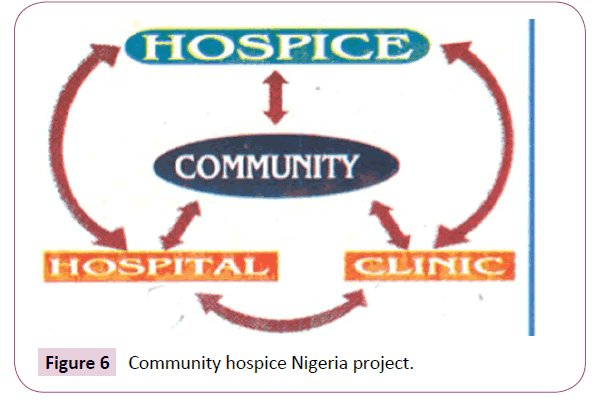
At the community level, the University College Hospital Ibadan team (CPCN) recently trained primary health care workers. Scaling up palliative care to the community is quite daunting with no support judging with the low success at the governmental level. The Community Hospice Nigeria project decided to take the bull by the horns to provide sensitization, advocacy, education training to the health care workers and the community at large besides providing quality palliative and End of life care at accessible at the grass-root level (Figure 6).
Figure 6: Community hospice Nigeria project.
Community Hospice Nigeria Project
The slow pace of palliative care development at both the tertiary and secondary tiers of health as a result of government bottleneck bureaucracy prompted me to explore community-based hospice palliative care service Project - (Community Hospice Nigeria – www.communityhospicenigeria.com).
Many elderly demented and geriatric patients are abandoned at home including stroke patients during the working hours until their family members joined them in the evening. Our Day Care Hospice facility has been providing a solace for this group of patients where they receive treatment and have the opportunity of interacting with their peer groups to reduce their boredom and loneliness at home.
The strategy is for the community hospice to serve as an interface between the patients in the community and the hospital besides home-based end of life-care.
This was the first stand-alone purposively built Hospice in Nigeria while on the other hand a Country like South Africa (60 million population) can boast of hundreds of standard hospices. Being a new project the community and many of the health care professionals are not aware or knowledgeable about the Hospice philosophy.
A lot of sensitization and advocacy still need to be done for the community to embrace and access the good death at home. The challenges are awesome as most of the patients present very late at advance disease stage with poverty and inability to pay. Other challenges include presentation to the hospice of the acutely ill patients and staff training and acquisition of pain management, palliative and end of life-care. There is a high staff turnover as the project is not very lucrative. Many patients owe bills and are bad debtors claiming that Hospice care is supposed to be free as obtains in developed countries.
Discussion and Conclusion
There is no doubt that the most populous African nation; Nigeria has a long way to go in terms of education, training, research and the provision of accessible and affordable pain, palliative and End of Life -Care to the citizenry. This paper had explored a minineeds assessment in the country and a larger much bigger needs assessment may be needed in the future.
“The harvest is ripe but the laborers are very few”, there is need for concerted efforts of both the local and International palliative care movement to improve the death and dying phenomenon in Nigeria. Approving the national palliative care policy, supporting the manpower development and other needed resources, could do this. This is an opportunity to invite all the stakeholders to come together and join us in scaling-up palliative care services in Nigeria as the adage says, “Service to Humanity is Service to God”.
References
- Oyebola FO (2005) Setting up palliative care in Nigeria-Appraisal of the challenges and new trends. Paper presented at the International Conference of Hospice and Palliative Care: Mind, Body, Spirit at the University of Cape Town, 2nd – 4th December 2005, South Africa.
- Adenipekun A, Onibokun A, Elumelu TN, Soyannwo OA (2005) Knowledge and attitudes of terminally ill patients and their family to palliative care and hospice services in Nigeria. Niger J Clin Pract 8: 19-22.
- Soyannwo O (2006) National Consultative Committee on Cancer.
- Oyebola FO (2006) The perception and needs assessment of home based palliative care among advanced disease patients attending Federal Medical Centre, Abeokuta, Nigeria.
- Oyebola FO (2006) Combined perception and needs assessment study of home based palliative care among patients with life-threatening diseases attending the Federal Medical Centre Abeokuta, Nigeria. Doctoral dissertation, University of Cape Town, South Africa.
- Oyebola FO, Igbinova J (2003) Federal Medical Centre Abeokuta, Hospice and Palliative Care Project. In: Palliative Care in Sub–Saharan Africa. Hardings R (ed), King`s College University, London.
- Oyebola FO (2010) Hospital based palliative care approach to HIV/AIDS: A Nigerian experience. Retrovirology. 7: 94.
- Oliver D, Olupitan D, Oyebola F (2011) Developing palliative care in Nigeria - A collaborative approach. J Palliat Care 18: 298-301.
- Alexander CS, Pappas G, Oyebola FO (2015) AIDS Relief Staff members: Implementation of HIV Palliative Care: Inter-professional education to improve patient outcomes in resource-constrained settings from 2004-2014. J Pain Symptom Manage 50: 350-361.
- Alexander CS, Pappas G, Henley Y, Kangalawe AK, Oyebola FO, et al. (2015) Pain management for persons living with HIV disease: An experience with interprofessional education in Nigeria. Am J Hosp Palliat Care 32: 555-362.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences